Stress fracture Treatment are small cracks in bones that develop gradually from repetitive strain, often affecting runners, athletes, dancers, or anyone who suddenly increases their activity levels. At first, the pain may feel like normal post-workout soreness, but it can worsen over time and interfere with daily activities. These injuries occur when bone remodeling cannot keep up with repeated microdamage, exceeding the bone’s repair capacity. If left untreated, a minor stress fracture can progress to a serious injury, potentially sidelining you for months. At DSK Hospitals, early diagnosis, proper treatment, and preventive measures, most stress fractures heal completely, allowing a safe and gradual return to activity.
What is a Stress Fracture?
- A stress fracture is a small crack or severe bruising in a bone that develops over time due to repetitive mechanical stress rather than a single traumatic event. These injuries are often referred to as overuse fractures, hairline fractures, or fatigue fractures because they typically result from repeated loading such as running, jumping, or marching that exceeds the bone’s ability to repair microdamage.
- Under normal conditions, healthy bone undergoes a constant cycle of remodeling, where microscopic damage is repaired as part of daily activity. However, when the bone is subjected to frequent or increased impact without enough time for recovery, microcracks accumulate faster than the body can mend them. This imbalance eventually leads to a stress fracture.
- Stress fractures most commonly occur in weight‑bearing bones of the lower body, such as the tibia (shin bone), metatarsals (foot bones), and fibula, but they can also affect the hip, pelvis, and other areas subjected to repetitive force.
- Unlike acute fractures caused by a one‑time injury, stress fractures develop gradually and may initially cause mild discomfort that worsens with continued activity. Early diagnosis and appropriate management are crucial, as untreated stress fractures can progress and lead to more serious bone injury.
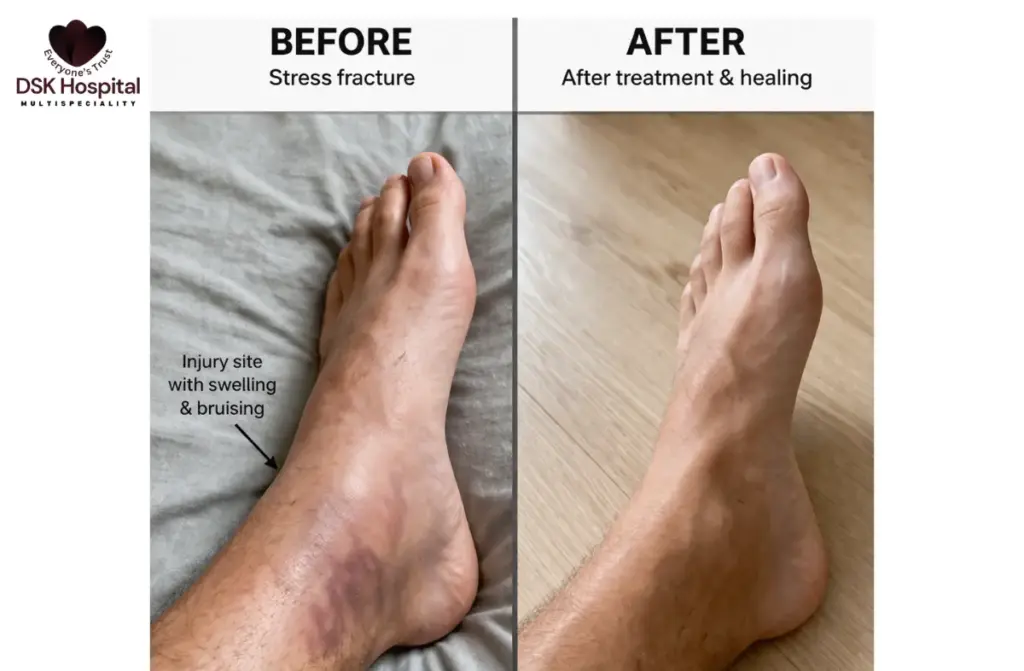
Common Locations
- Stress fractures can affect various bones, depending on the type of activity and load distribution:
- Foot (metatarsals): Common in runners and dancers.
- Shin (tibia): One of the most frequent sites for runners.
- Heel: Often seen in jumpers and athletes performing high-impact movements.
- Hip and pelvis: More common in long-distance runners and military recruits.
Key Characteristics
- Develop gradually, rather than suddenly.
- Result from repetitive activity rather than acute trauma.
- Difficult to detect early without imaging.
Causes & Risk Factors
Stress fractures occur when the physical stress placed on the bone exceeds the body’s ability to repair and adapt. Understanding the causes of stress fractures is important for prevention and effective stress fracture treatment. Certain risk factors increase the likelihood of developing stress fracture symptoms, including low bone density or poor nutrition.
Common Causes
Overuse and repetitive motion: In orthopaedics, stress fractures are considered common sports injuries, often caused by overuse and repetitive motion, such as running or jumping, which increases bone stress
Sudden increase in activity: Rapid escalation in intensity, duration, or frequency.
Poor exercise technique: Incorrect form or biomechanical imbalances.
Hard training surfaces: Concrete or other rigid surfaces increase impact stress.
Improper footwear: Worn-out or unsupportive shoes fail to cushion impact forces.
Risk Factors
Several stress fracture causes make certain individuals more prone, including rapid increase in activity and poor footwear.
- Low bone density or osteoporosis.
- Vitamin D deficiency, which impairs calcium absorption.
- Poor nutrition, especially insufficient protein and calcium.
- Previous injuries, which may compromise structural integrity.
- Foot structure abnormalities, such as high arches or flat feet.
Pro Tip: Increase your training intensity by no more than 10% per week to minimize injury risk.
Symptoms of a Stress Fracture
Stress fracture symptoms often develop slowly and intensify with continued activity. Recognizing early symptoms allows for timely stress fracture treatment, preventing progression to more serious fractures. Pain from a tibia stress fracture often worsens during running or jumping activities.
Key Symptoms
- Pain concentrated directly over the affected bone.
- Swelling and tenderness over the affected bone.
- Pain that occurs during activity but improves with rest.
- Persistent pain even at rest in advanced cases.
When to See a Doctor
Seek professional evaluation if you notice:
- Pain that persists even when inactive.
- Swelling that does not subside.
- Pain worsening over time.
- Difficulty bearing weight on the affected limb.
- History of previous stress fractures.
Early diagnosis prevents minor stress fractures from progressing into more serious injuries.
How Stress Fractures are Diagnosed
Diagnosis is essential to differentiate stress fractures from other conditions, such as shin splints or tendonitis. Doctors check for tenderness and swelling along the shin when a tibia stress fracture is suspected.
Step 1: Physical Examination
A doctor will assess:
- Location and intensity of pain.
- Recent activity history.
- Tenderness or swelling around the bone.
Step 2: Imaging Tests
- X-rays: Typically the first imaging step. However, stress fractures may not be visible for the first 2–3 weeks.
- MRI: Highly sensitive and effective in detecting early-stage stress fractures.
- Bone scan: Used selectively when MRI is not available or for multiple suspected sites.
Stress Fracture Treatment Options
Stress Fracture Treatment varies depending on the severity, location, and type of fracture. Most stress fractures heal without surgical intervention.
Non-Surgical Treatment
1. Rest and Activity Modification
Reducing or modifying activity is critical. Avoid running or high-impact exercises until pain subsides.
2. Ice Therapy
Applying ice can help reduce pain and swelling.
3. Protective Footwear or Walking Boot
Immobilization or supportive footwear may be recommended to reduce stress on the bone.
4. Crutches
Used in more severe cases to prevent weight-bearing on the affected bone.
5. Pain Management
Mild pain can be managed with ice and rest. In some cases, over-the-counter medications may be recommended by a doctor.
6. Nutritional Support
Adequate intake of calcium, vitamin D, and protein is crucial for bone repair and overall recovery.
7. Low-Impact Alternatives
During recovery, low-impact exercises maintain fitness without stressing the injured bone:
- Swimming
- Cycling
- Elliptical workouts
Note: Returning to high-impact activity prematurely may interfere with recovery or result in a serious fracture.
Surgical Treatment
Operations are generally unnecessary, except in cases such as:
- High-risk fractures (e.g., certain hip fractures).
- Cases of delayed healing or non-union.
- Professional athletes require faster recovery timelines.
Advanced surgical options may include bone stimulators or procedures using screws/pins to stabilize the bone.
Rehabilitation & Recovery
Recovery typically spans 6–8 weeks, but timelines vary depending on fracture severity and patient compliance. A structured rehabilitation program is an essential part of stress fracture treatment, helping patients regain strength and return to activity safely.
Recovery Timeline
- Weeks 1–2: Rest, pain control, and minimal activity.
- Weeks 3–4: Begin light movement and low-impact activity.
- Weeks 5–6: Incorporate strength and flexibility exercises.
- Weeks 7–8: Gradual return to normal or sport-specific activities.
Recommended Rehabilitation Exercises
- Calf raises
- Resistance band ankle exercises
- Core strengthening workouts
- Balance and stability training
These exercises help restore strength, prevent muscle atrophy, and improve joint stability.
Stress Fracture vs. Shin Splints
Proper diagnosis is critical because treatment differs:
- Stress Fracture: Localized pain, worsens over time, tenderness at a specific point.
- Shin Splints: Diffuse pain along the shin, often improves with rest and reduced activity.
- Identifying the correct condition ensures effective treatment and prevents complications.
Prevention
Preventing stress fractures requires a combination of training strategy, proper equipment, nutrition, and body awareness. Being aware of common stress fracture causes helps athletes adjust training and avoid overuse injuries. Monitoring for recurring stress fracture symptoms ensures timely treatment and safe return to activity.
Top Strategies
- Follow the 10% rule: Gradually increase training intensity.
- Wear proper footwear: Ensure adequate cushioning and support.
- Cross-train: Reduce repetitive impact on the same bones.
- Maintain a balanced diet: Support bone health with calcium, vitamin D, and protein.
- Strengthen muscles: Strong muscles absorb impact and reduce bone stress.
- Avoid hard surfaces: Prefer tracks or softer terrain for high-impact activities.
Quick Tip: Replace running shoes every 300–500 miles to maintain proper cushioning and support.
Conclusion
Stress fracture treatment is essential for these common yet highly manageable injuries. Successful recovery depends on early recognition, appropriate care, and patient compliance. Ignoring symptoms or returning to high-impact activity too soon can lead to serious complications, including complete fractures or chronic pain. Prioritizing rest, following a structured stress fracture treatment plan, gradually returning to activity, and maintaining proper nutrition to support bone health are key steps for a safe and effective recovery. By taking these measures, individuals can heal fully and return to their active lifestyle while minimizing the risk of recurrence. Read Also : How to improve bone health


